Beyond Blood Sugar: How Incretin Peptides Are Redefining Metabolic Health
Abstract
Multifunctional incretin peptides are revolutionizing the treatment landscape for type 2 diabetes and obesity. Unlike traditional therapies that target a single metabolic pathway, these innovative peptides are designed to activate multiple receptors—such as GLP-1, GIP, and glucagon—delivering synergistic effects on blood glucose control, weight loss, and overall metabolic health. Dual agonists like tirzepatide have already shown superior results in clinical trials, while triple agonists are demonstrating promising benefits in early-stage studies. These therapies not only improve insulin sensitivity and reduce fat storage but may also address related conditions such as NAFLD and cardiovascular disease. While challenges like tolerability and delivery remain, the future of incretin-based therapy is bright, with ongoing research pushing the boundaries of what’s possible in metabolic disease management. This blog explores the science, clinical data, and future potential of multifunctional incretin peptides.
New Solutions for Old Problems: Incretin Peptides in Diabetes and Obesity Care
Type 2 diabetes and obesity are among the most widespread and challenging health issues of our time, affecting hundreds of millions of people around the globe. Despite a wide range of available treatments, many patients continue to struggle with poor blood sugar control, weight gain, and related health complications. This growing need for more effective therapies has led to increased interest in a powerful class of molecules known as incretin peptides.
Incretin peptides, such as GLP-1 (glucagon-like peptide-1) and GIP (glucose-dependent insulinotropic polypeptide), are naturally occurring hormones that help regulate insulin secretion and glucose metabolism after meals. They form the foundation of some of today’s most effective type 2 diabetes and anti-obesity treatments—particularly GLP-1 receptor agonists, which have shown significant success in both lowering blood sugar and promoting weight loss.

Now, a new generation of therapies is emerging: multifunctional incretin peptides. These innovative compounds are designed to activate multiple hormone receptors at once, offering more comprehensive benefits for blood glucose control, weight reduction, and overall metabolic health.
Understanding Incretins: How GLP-1 and GIP Regulate Metabolism
Incretin hormones are key regulators of blood glucose levels and play a crucial role in maintaining metabolic balance. The two primary incretins are GLP-1 (glucagon-like peptide-1) and GIP (glucose-dependent insulinotropic polypeptide), both of which are released from the gut in response to food intake. Their main function? To enhance insulin secretion from the pancreas—but only when blood sugar levels are elevated. This smart, glucose-dependent action helps reduce the risk of hypoglycemia, a common side effect of many diabetes treatments.
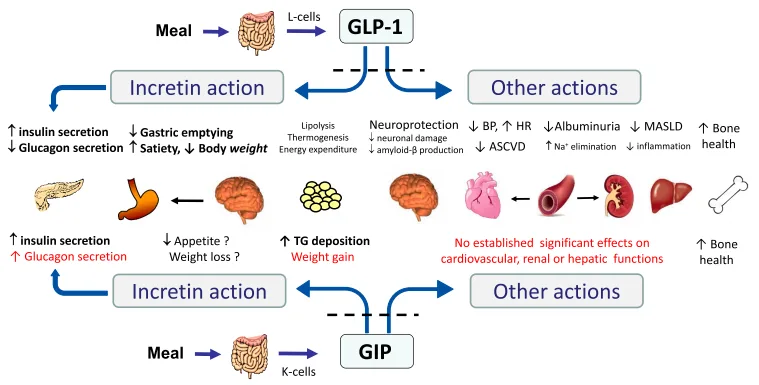
Among the two, GLP-1 has received the most attention in clinical medicine. GLP-1 not only boosts insulin secretion but also slows gastric emptying, reduces appetite, and supports weight loss—making GLP-1 receptor agonists a popular and effective option for both type 2 diabetes and obesity management.
On the other hand, GIP has long been overlooked due to inconsistent clinical results. However, recent research suggests that when combined with other hormones like GLP-1, GIP may actually enhance metabolic outcomes, paving the way for its resurgence in modern diabetes therapies.
Together, these hormones form the basis for a new class of treatments that target multiple metabolic pathways simultaneously—offering a more holistic approach to managing chronic metabolic diseases.
Beyond Single Targets: The Rise of Dual and Triple Incretin Agonists
While single-hormone therapies like GLP-1 receptor agonists have shown impressive results, researchers are now exploring a more powerful approach: multifunctional incretin peptides. These next-generation therapeutics are engineered to activate two or more hormone receptors simultaneously, offering synergistic benefits that go beyond what single agonists can achieve.
One of the most promising innovations in this space is the development of dual agonists, such as those targeting both GLP-1 and GIP receptors. A standout example is tirzepatide, the first FDA-approved GLP-1/GIP dual agonist. In clinical trials, tirzepatide has demonstrated superior glucose control and greater weight loss compared to GLP-1 monotherapy—making it a breakthrough option for patients struggling with both type 2 diabetes and obesity.
In parallel, scientists are also investigating GLP-1/glucagon dual agonists, which show potential in increasing energy expenditure and promoting fat loss—further addressing obesity and associated metabolic conditions.
Even more exciting is the rise of triple agonists, which simultaneously target GLP-1, GIP, and glucagon receptors. These multifunctional peptides are currently in clinical development and have shown remarkable metabolic improvements in preclinical studies, including better blood glucose regulation, reduced liver fat, and significant weight loss.
As these multifunctional incretin therapies continue to evolve, they are redefining the landscape of metabolic disease management by offering a more comprehensive, multi-targeted treatment strategy.
How Multifunctional Peptides Deliver Synergistic Metabolic Benefits
The real power of multifunctional incretin peptides lies in their ability to target multiple metabolic pathways at once, unlocking broader therapeutic effects than traditional treatments. By activating combinations of receptors—typically GLP-1, GIP, and glucagon receptors—these peptides deliver synergistic effects across several key areas of metabolism.
First, they enhance insulin secretion in a glucose-dependent manner, which helps lower blood sugar levels more effectively and safely. This is especially important for patients with type 2 diabetes, where insulin production and sensitivity are often impaired.
Second, they suppress appetite and promote feelings of fullness, leading to a natural reduction in food intake. This effect is largely driven by GLP-1 receptor activation in the brain and gut, contributing significantly to weight loss outcomes.
Third, when the glucagon receptor is also activated—as in dual or triple agonist designs—it can increase energy expenditure and help break down fat stores. This is particularly beneficial for individuals struggling with obesity or non-alcoholic fatty liver disease (NAFLD).
In addition to glucose and weight control, early evidence suggests that multifunctional incretin therapies may also provide cardiovascular and kidney protection, addressing the complications often associated with diabetes and obesity.
In short, these peptides work by harmonizing hormonal signals, helping the body regulate blood sugar, body weight, and lipid metabolism more effectively than ever before.
Tirzepatide and Beyond: Clinical Breakthroughs in Incretin Therapy
The clinical impact of multifunctional incretin peptides is already being felt, with real-world data showing transformative results—especially with dual agonists like tirzepatide. In head-to-head clinical trials, tirzepatide has consistently outperformed existing GLP-1 receptor agonists in both blood glucose control and weight reduction.

Patients treated with tirzepatide experienced HbA1c reductions of up to 2.5% and average weight losses exceeding 20% in some studies—outcomes that rival or even surpass those seen with bariatric surgery. These results have positioned tirzepatide as a game-changing therapy for individuals with type 2 diabetes and obesity.
Meanwhile, triple agonists—targeting GLP-1, GIP, and glucagon receptors—are showing great promise in early-phase clinical trials. Preclinical data suggests that these next-generation peptides may deliver even greater metabolic benefits, including improved insulin sensitivity, enhanced fat oxidation, and reductions in liver fat—making them potential therapies for conditions like NAFLD/NASH.
As research advances, these peptides are not only redefining treatment expectations but also opening doors to more personalized and effective metabolic care, with several new candidates progressing rapidly through the clinical pipeline.
What’s Next? Challenges, Innovations, and the Future of Metabolic Treatment
While multifunctional incretin peptides represent a breakthrough in treating type 2 diabetes and obesity, several challenges remain. Balancing the activation of GLP-1, GIP, and glucagon receptors is complex—overstimulating one pathway, particularly the glucagon receptor, can reduce effectiveness or cause side effects. Common tolerability issues like nausea and vomiting, especially early in treatment, may also impact patient adherence.
Currently, most therapies require subcutaneous injections, which may be inconvenient for some. However, advances in oral formulations and long-acting injectables are underway to improve accessibility and ease of use.
Despite these hurdles, the future of metabolic disease therapy looks promising. Dual agonists like tirzepatide have already shown superior results in controlling blood sugar and reducing weight. Emerging triple agonists may offer even broader benefits—targeting not just diabetes and obesity, but also conditions like non-alcoholic fatty liver disease (NAFLD) and cardiovascular risk.
As research progresses, multifunctional incretin peptides are set to reshape the standard of care for millions worldwide. Their ability to tackle multiple metabolic challenges simultaneously positions them as a key innovation in the future of personalized, high-impact metabolic therapy.
 LinkPeptide
LinkPeptide