Exploring the Role of Neuropeptides in Orofacial Pain: Implications for Future Treatments
Abstract
Orofacial pain, a prevalent and often debilitating condition, involves complex mechanisms that remain inadequately addressed by current therapeutic options. Neuropeptides, small protein-like molecules involved in pain regulation, have emerged as key mediators in the development and modulation of orofacial pain. This review explores the roles of various neuropeptides, including Calcitonin Gene-Related Peptide (CGRP), Substance P (SP), Opioid Peptides (OP), Galanin (GAL), and others, in the trigeminal system. These neuropeptides contribute to neurogenic inflammation, pain sensitization, and both the initiation and persistence of pain. Their diverse pro-nociceptive and anti-nociceptive effects highlight their potential as therapeutic targets. Advances in neuropeptide-based therapies, such as CGRP antagonists and SP receptor antagonists, offer promising new avenues for treating conditions like temporomandibular joint disorders, dental pain, and migraines. However, challenges in targeting these pathways remain, requiring continued research to optimize their clinical applications and improve pain management strategies.
Understanding Orofacial Pain and Its Challenges
Orofacial pain refers to any discomfort or pain affecting the mouth, jaws, face, or surrounding structures. It encompasses a wide range of conditions, including dental pain, temporomandibular joint (TMJ) disorders, trigeminal neuralgia, and myofascial pain. This type of pain affects a significant portion of the population, with prevalence rates ranging from 10% to 26%. Orofacial pain can arise from numerous causes, including inflammatory conditions, nerve damage, or injury to the muscles, bones, or soft tissues of the face. It is often complex, with both physical and emotional components, making it a significant medical and social issue.
The clinical management of orofacial pain presents a challenge due to its multifactorial nature and the limited effectiveness of current treatments. Understanding the underlying mechanisms of pain, particularly at the molecular level, is crucial for developing more targeted therapies. Neuropeptides, which are small protein-like molecules that transmit signals in the nervous system, play a pivotal role in regulating pain and inflammation. Their involvement in orofacial pain processes—ranging from the initiation of inflammatory responses to the modulation of sensory pathways—highlights their potential as therapeutic targets. In this blog, we will delve into the role of neuropeptides in orofacial pain, aiming to better understand their functions and their potential for improving pain management strategies in both clinical and research settings.
The Role of Neuropeptides in Orofacial Pain: Key Players Unveiled
Neuropeptides are small protein-like molecules that act as neurotransmitters in the nervous system. They are produced by neurons and play a critical role in transmitting signals between nerve cells. Unlike classical neurotransmitters, which act on receptors located on the surface of cells, neuropeptides can have a broader and more lasting effect by influencing the activity of both neurons and surrounding cells, such as glial cells and immune cells. Neuropeptides are involved in regulating a variety of physiological functions, including pain perception, stress responses, immune regulation, and the modulation of inflammation. In the context of orofacial pain, neuropeptides are key players in the initiation, amplification, and maintenance of pain signals in response to injury or inflammation.
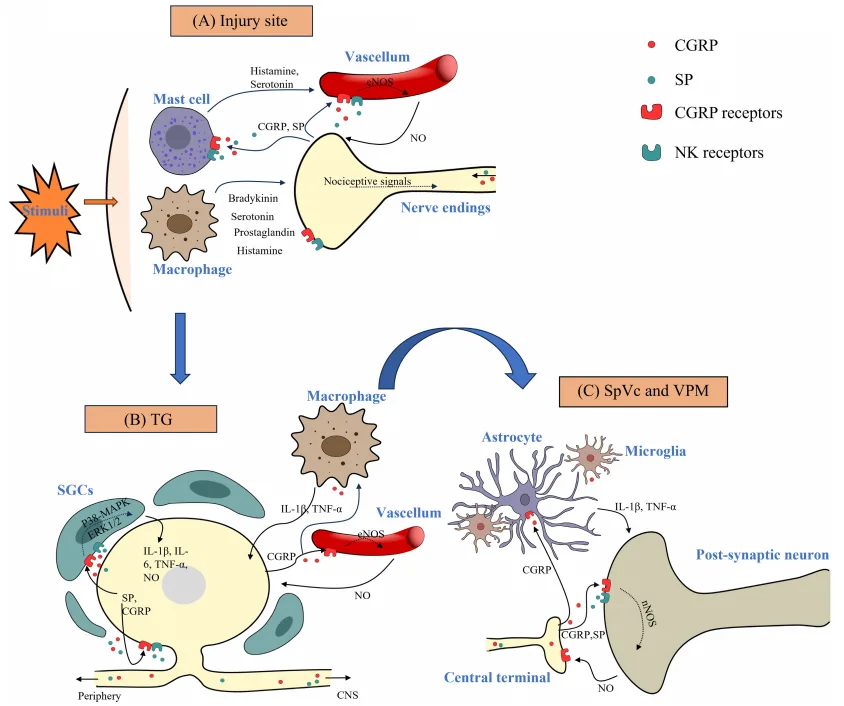
Calcitonin Gene-Related Peptide (CGRP)
CGRP is a key neuropeptide in orofacial pain, highly expressed in the trigeminal system, which controls sensation in the face. As a potent vasodilator, CGRP widens blood vessels and increases blood flow, playing a significant role in neurogenic inflammation. It promotes the release of inflammatory mediators, sensitizing nociceptors (pain receptors) and making the affected area more sensitive to pain. CGRP is crucial in conditions like temporomandibular joint disorders and migraine, where it amplifies pain signals and perpetuates pain cycles. Its ability to initiate and maintain both peripheral and central sensitization makes it a vital therapeutic target.
Substance P (SP)
Substance P is widely distributed throughout the trigeminal system and plays a major role in the inflammatory pain response. When released, SP binds to receptors on blood vessels, neurons, and immune cells, causing vasodilation and increasing vascular permeability. This facilitates the movement of inflammatory cells to the injury site, exacerbating pain. SP is particularly involved in the early stages of pain, sensitizing nerve fibers and amplifying pain signals. Elevated SP levels are often found in conditions like pulpitis and temporomandibular joint (TMJ) pain, linking it to the development of orofacial pain.
Opioid Peptides (OP)
Opioid peptides, including endorphins, enkephalins, and dynorphins, are natural analgesics. They function by binding to opioid receptors on neurons and glial cells, inhibiting pain signal transmission. In orofacial pain, these peptides are released in response to injury or inflammation, alleviating pain by dampening the excitability of pain-sensing neurons. Opioid peptides act both peripherally and centrally, modulating the trigeminal system’s sensitivity to painful stimuli. Research suggests that enhancing the body’s own opioid systems may offer a safer alternative to synthetic opioids, which carry risks of dependency and side effects.
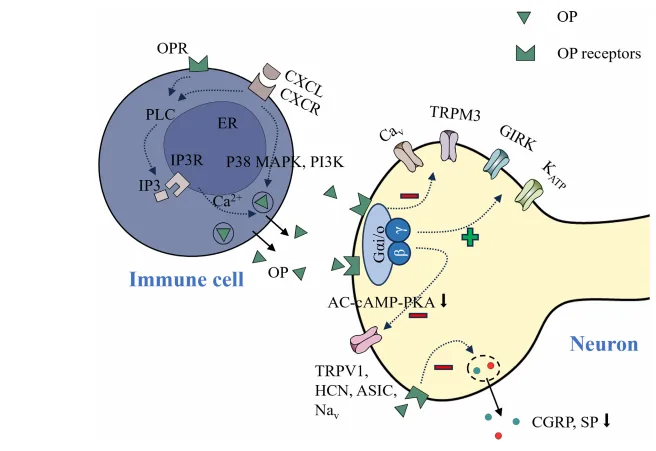
Galanin (GAL)
Galanin has dual effects on pain, acting as an analgesic or nociceptive agent depending on its concentration and receptor activation. In the trigeminal system, galanin generally has an antinociceptive (pain-relieving) effect by inhibiting pain transmission. However, at high concentrations, it may also contribute to pain sensitivity. Galanin interacts with other neuropeptides and inflammatory mediators to either reduce or enhance pain, making its role in orofacial pain modulation complex. Understanding galanin’s precise mechanisms is key to developing targeted therapies that maximize its analgesic effects.
Other Neuropeptides
Neuropeptide Y (NPY) plays a role in regulating pain sensitivity and inflammation, with some studies showing it inhibits nociceptor activation. Neurokinin A (NKA), like SP, is involved in pain responses, especially in dental pain and neurogenic inflammation. Oxytocin (OXT), known for its roles in childbirth, has analgesic effects in orofacial pain, particularly in nerve injury. Orexin A (OrxA) modulates pain pathways and may suppress nociceptive transmission. Vasoactive Intestinal Peptide (VIP) is involved in the inflammatory processes that exacerbate orofacial pain, particularly in periodontal disease. These neuropeptides contribute to a complex network of signaling mechanisms regulating orofacial pain, offering potential targets for future therapies.
Together, these neuropeptides contribute to the complex network of signaling mechanisms that regulate orofacial pain, offering potential targets for future therapeutic interventions aimed at providing more effective and targeted pain relief.
Neuropeptides as Targets for Pain Management
As research into orofacial pain mechanisms advances, the potential for targeting neuropeptides in therapeutic interventions becomes increasingly evident. Neuropeptides, such as CGRP, Substance P (SP), Opioid Peptides (OP), and Galanin (GAL), play pivotal roles in modulating pain and inflammation. This understanding has led to the exploration of various neuropeptide agonists, antagonists, and analogues as potential treatment options. These substances can either enhance or block the actions of specific neuropeptides, offering a promising avenue for more effective, targeted therapies in managing orofacial pain.
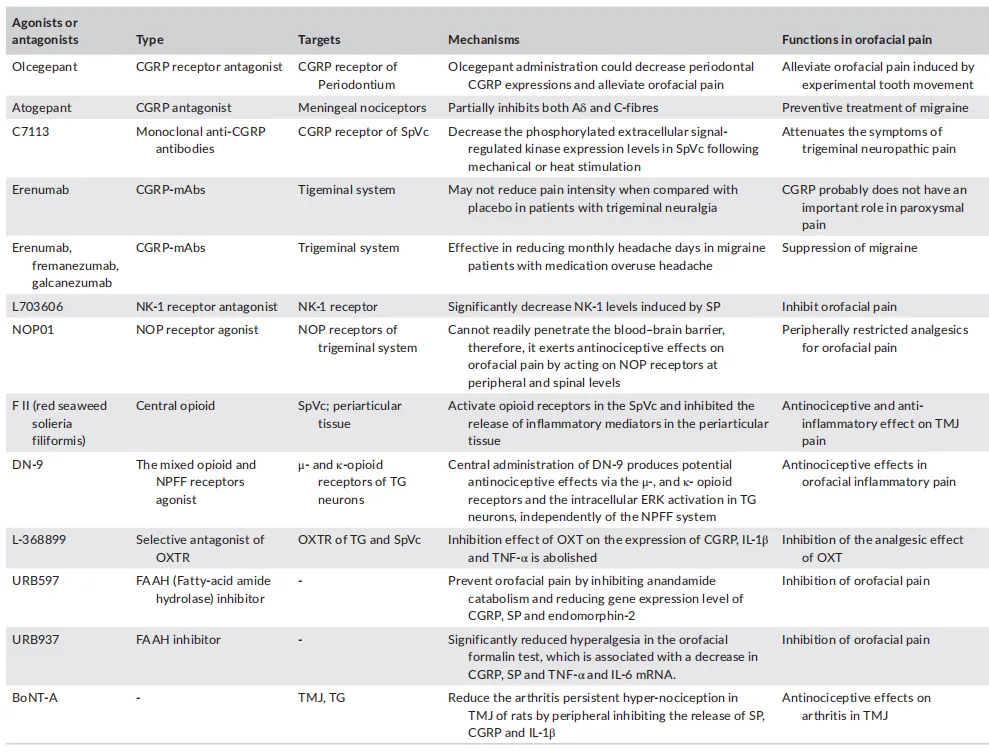
CGRP Antagonists and Monoclonal Antibodies
CGRP (Calcitonin Gene-Related Peptide) is extensively studied in orofacial pain, particularly in migraine and temporomandibular joint (TMJ) disorders. CGRP antagonists, such as erenumab, fremanezumab, and galcanezumab, have shown effectiveness in reducing pain frequency and severity in migraine patients. These drugs work by blocking CGRP receptors or neutralizing the peptide itself, preventing the inflammatory and pain-enhancing effects of CGRP. Additionally, studies have shown that CGRP antagonists can alleviate orthodontic pain and trigeminal neuropathic pain. However, their use in treating trigeminal neuralgia has yielded mixed results, highlighting the need for more research to determine their effectiveness in various pain types.
Substance P Receptor Antagonists
Substance P (SP) is a critical neuropeptide in the inflammatory pain response, particularly in the orofacial region. SP receptor antagonists, which target the NK1 receptors, have demonstrated promise in reducing pain and inflammation in conditions like TMJ disorders and pulpitis. Blocking the interaction between SP and its receptors helps alleviate hypersensitivity in the trigeminal system, reducing peripheral and central sensitization. While promising, SP receptor antagonists are still in the early stages of clinical use, and further studies are needed to evaluate their safety and long-term effectiveness.
Opioid Peptides and Their Agonists
Opioid peptides, including endorphins and enkephalins, are natural analgesics that bind to opioid receptors in the nervous system, inhibiting pain transmission. Opioid receptor agonists, such as β-endorphins and enkephalin analogs, can effectively reduce pain in the trigeminal system. However, the use of opioids—especially exogenous opioids—poses significant risks, including dependency and side effects. Research is focused on developing safer, more targeted opioid peptide agonists that provide pain relief without the addictive potential of traditional opioids, with advances in peripherally acting opioids showing promise.
Galanin and Its Modulators
Galanin plays a complex role in pain modulation, acting either as an analgesic or nociceptive agent depending on its concentration and receptor activation. Galanin receptor agonists, especially targeting GalR1 and GalR2 receptors, have shown potential as pain-relieving agents. At low concentrations, GalR2 activation may promote pain, while higher concentrations offer analgesic effects. Researchers are exploring selective GalR2 agonists to help reduce pain while minimizing pro-nociceptive effects. Additionally, galanin receptor antagonists are being studied to block galanin’s pro-nociceptive effects, although more research is needed to assess their clinical utility in orofacial pain.
Neuropeptide Y (NPY) and Other Neuropeptides
Neuropeptide Y (NPY) receptor agonists show promise in modulating orofacial pain, with some studies indicating they can inhibit nociceptor activation and reduce the release of pain-related neuropeptides like CGRP and SP. NPY antagonists are also being explored, though this research is in the early phases. Other neuropeptides, such as Neurokinin A (NKA) and Hemokinin-1 (HK-1), are also being investigated for their roles in pain modulation and their potential as therapeutic targets in orofacial pain.
Advancing Neuropeptide-Based Therapies for Orofacial Pain
While targeting neuropeptides for pain management holds significant promise, several challenges remain. One of the main obstacles is the complexity of neuropeptide interactions, as the same neuropeptide can have different effects depending on its concentration, receptor subtype, and the stage of the pain process. Additionally, drug delivery remains a key concern. Many neuropeptide-targeting drugs face difficulty crossing the blood-brain barrier or achieving the necessary local concentration at the pain site without systemic side effects.
Despite these challenges, the development of novel neuropeptide-based therapies continues to progress. New delivery methods, such as topical formulations, intranasal sprays, or local injections, are being explored to maximize the efficacy of these treatments. As more is understood about the specific roles of various neuropeptides in orofacial pain, researchers are optimistic that neuropeptide-based therapies will offer a more targeted, effective, and safer alternative to current pain management options. The future of neuropeptide research promises to bring innovative solutions for those suffering from chronic and acute orofacial pain, with the potential for more personalized and effective treatments.
Unlocking the Potential of Neuropeptides in Pain Relief
In conclusion, neuropeptides play a pivotal role in the development and modulation of orofacial pain, influencing both the initiation and maintenance of pain through mechanisms such as neurogenic inflammation and pain sensitization. Key neuropeptides like CGRP, Substance P, opioid peptides, and galanin act on the trigeminal system, shaping the perception of pain in the orofacial region. Their dual pro-nociceptive and anti-nociceptive effects make them significant targets for therapeutic intervention.
The ongoing research into neuropeptide-based therapies, including CGRP antagonists, SP receptor antagonists, and opioid peptide agonists, holds promise for improving the management of conditions such as temporomandibular joint disorders, dental pain, and migraines. However, challenges remain in targeting these neuropeptides effectively without causing adverse effects.
As research continues to evolve, neuropeptides offer exciting potential for novel treatments that can provide more precise, effective pain relief. Advancing our understanding of their roles in orofacial pain will be essential in developing innovative therapies that can address the diverse needs of patients and improve their quality of life.
 LinkPeptide
LinkPeptide