From Obesity to Metabolic Health: Why Retatrutide Is a Game-Changer
Abstract
Obesity and type 2 diabetes have become global health crises, fueling complications such as cardiovascular disease, fatty liver disease, and metabolic syndrome. While existing peptide-based therapies like semaglutide and tirzepatide have reshaped treatment, many patients still face incomplete results or intolerable side effects. Retatrutide, a next-generation triple-agonist peptide developed by Eli Lilly, offers a new approach by targeting GLP-1, GIP, and glucagon receptors simultaneously. This unique mechanism delivers unprecedented outcomes in clinical trials, including up to 24.2% body weight reduction, significant HbA1c improvements, reversal of prediabetes, and dramatic reductions in liver fat. Early findings also suggest potential benefits in systemic inflammation, kidney function, and metabolic syndrome. Though gastrointestinal side effects and cardiovascular considerations remain under investigation, retatrutide stands as a promising innovation that could redefine the future of weight management and metabolic care, positioning peptide therapies at the forefront of modern medicine.
The Global Metabolic Health Crisis
Obesity and type 2 diabetes are among the most urgent health crises of our time. Today, more than one billion people worldwide live with obesity, and over 500 million are affected by diabetes. These conditions often go hand in hand, fueling complications such as cardiovascular disease, fatty liver disease, and metabolic syndrome. Together, they shorten lives, reduce quality of life, and place a growing burden on healthcare systems worldwide.
In recent years, peptide-based medicines have transformed how we approach these challenges. GLP-1 receptor agonists like semaglutide (Ozempic®, Wegovy®) and the dual GLP-1/GIP agonist tirzepatide (Mounjaro®) have delivered significant advances in weight management and blood sugar control. Yet for many patients, progress is incomplete. Weight loss may plateau, blood glucose targets remain out of reach, or side effects limit long-term use.

This is why retatrutide has generated so much excitement. As a next-generation triple-action peptide, it works by targeting GLP-1, GIP, and glucagon receptors together—three critical pathways in metabolism. This innovative approach aims to deliver deeper, more durable results across weight reduction, glycemic control, and overall metabolic health. With clinical studies already showing remarkable outcomes, retatrutide may soon redefine the future of obesity and diabetes care.
What Makes Retatrutide Different? The Triple-Agonist Advantage
What sets retatrutide apart from today’s weight-loss and diabetes therapies is its unique triple-agonist mechanism. Unlike semaglutide, which activates only the GLP-1 receptor, or tirzepatide, which targets both GLP-1 and GIP, retatrutide engages three key metabolic receptors simultaneously:
- GLP-1 receptor – curbs appetite, slows gastric emptying, and lowers blood sugar.
- GIP receptor – enhances insulin secretion and supports weight loss when paired with GLP-1 activity.
- Glucagon receptor – boosts energy expenditure and fat burning, helping sustain long-term weight reduction.
By combining these pathways, retatrutide amplifies metabolic effects that no single or dual agonist can fully achieve. This synergy is what makes it so promising for people who have struggled to lose weight or control blood sugar despite current medications.

In early clinical studies, retatrutide has delivered unprecedented weight loss—up to 24.2% of body weight in less than a year—while also improving blood pressure, cholesterol, and liver fat content. These multi-dimensional benefits suggest that retatrutide is more than a weight-loss drug; it is a comprehensive metabolic therapy.
For patients and healthcare providers, the appeal is clear: retatrutide may finally address the full spectrum of metabolic dysfunction—from obesity and diabetes to fatty liver disease—offering a treatment option that is both broader in scope and more powerful in effect.
Groundbreaking Results from Clinical Trials
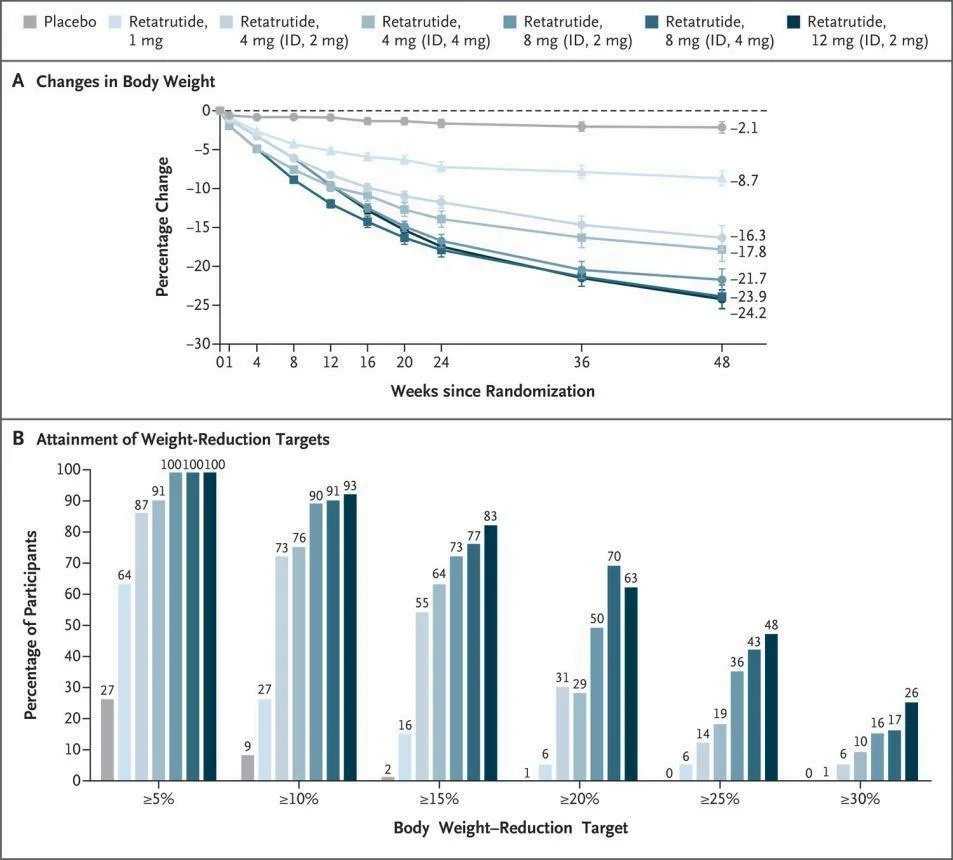
The promise of retatrutide is not just theoretical—it is already supported by compelling clinical evidence. In a landmark Phase 2 trial, patients receiving the highest dose of retatrutide (12 mg) achieved an average weight loss of 24.2% after 48 weeks. To put that in perspective, this level of weight reduction is comparable to what can be seen after some forms of bariatric surgery, but achieved through a peptide-based therapy. Even lower doses produced meaningful results, highlighting its strong, dose-dependent effect.
For people living with type 2 diabetes, the benefits go beyond weight loss. Clinical trials have shown that retatrutide can lower HbA1c (a key marker of blood sugar control) by more than 2%, a remarkable improvement compared to many existing treatments. Importantly, in one study, nearly three-quarters of participants with prediabetes returned to normal blood sugar levels, suggesting that retatrutide may help not only manage but even reverse early metabolic dysfunction.
Retatrutide has also demonstrated promising results in liver health. In patients with metabolic dysfunction-associated steatotic liver disease (MASLD), more than 85% experienced resolution of liver fat accumulation, with reductions of over 70% in fat content. This makes retatrutide one of the first therapies to show real potential in addressing this fast-growing condition, which is often linked to obesity and diabetes.
Beyond these headline outcomes, studies also report improvements in blood pressure, cholesterol, and insulin sensitivity, painting a picture of a therapy that supports the body’s entire metabolic system. Taken together, these results position retatrutide as a breakthrough in comprehensive metabolic care, moving far beyond the limitations of current weight-loss and diabetes medications.
Balancing Benefits with Safety
Like all powerful therapies, retatrutide comes with considerations that patients and clinicians must weigh carefully. The most common side effects reported in clinical trials are gastrointestinal issues such as nausea, vomiting, and diarrhea. These effects are generally mild to moderate and tend to improve over time, especially when dosing is adjusted gradually. Still, they remain an important factor in patient comfort and adherence.
Another area of attention is cardiovascular safety. Some participants in early studies experienced slight increases in heart rate or mild rhythm disturbances. While these findings have not been linked to serious adverse outcomes so far, they highlight the need for long-term safety studies, which are currently underway in Phase 3 trials.
It’s worth noting that retatrutide’s safety profile appears broadly consistent with other peptide-based treatments like semaglutide and tirzepatide, which also carry gastrointestinal considerations. What sets it apart is the potential for even greater efficacy, which may outweigh these manageable side effects for many patients.
In short, while retatrutide looks highly promising, careful monitoring and more data are needed before it becomes widely available. For patients, this means a future option that balances powerful metabolic benefits with a safety profile that continues to be refined.
Looking Ahead: Why Retatrutide Matters for the Future of Peptide Medicine
Retatrutide is more than just another entry in the field of weight-loss drugs—it represents a new era in peptide-based medicine. By combining three powerful mechanisms in one therapy, it demonstrates how multi-receptor peptides can deliver broader, more durable results than ever before. This approach doesn’t just tackle obesity or diabetes in isolation; it addresses the full spectrum of metabolic dysfunction, from blood sugar imbalance to fatty liver disease and systemic inflammation.
For patients, the implications are far-reaching. Retatrutide could provide a path to sustained weight loss, better blood sugar control, and improved liver and cardiovascular health—all within a single treatment. For those who have struggled with plateaus on existing medications, or who face multiple interconnected health issues, this kind of therapy may offer a more complete solution.
Beyond obesity and diabetes, researchers are already exploring how retatrutide might benefit conditions such as kidney disease, metabolic syndrome, and even age-related decline. By improving insulin sensitivity, reducing inflammation, and supporting energy metabolism, it aligns with broader goals in wellness and healthy aging—areas of growing interest for both patients and practitioners.
As Phase 3 studies progress and more data emerges, the excitement surrounding retatrutide will only grow. If approved, it could redefine the standard of care for millions worldwide. At Linkpeptide, we continue to follow such breakthroughs closely, reflecting our commitment to supporting innovation in peptide science.
Retatrutide may well be the therapy that bridges the gap between cutting-edge research and real-world transformation—signaling the future of personalized metabolic care.
Reference
Monis, A., & Maple, K. (2025). Retatrutide: A Promising Multimodal Peptide for Weight Management and Metabolic Health.
Jastreboff, A. M., Kaplan, L. M., Frías, J. P., Wu, Q., Du, Y., Gurbuz, S., … & Hartman, M. L. (2023). Triple–hormone-receptor agonist retatrutide for obesity—a phase 2 trial. New England Journal of Medicine, 389(6), 514-526.
https://doi.org/10.1016/B978-0-443-27370-4.00013-5
Ma, J., Hu, X., Zhang, W., Tao, M., Wang, M., & Lu, W. (2025). Comparison of the effects of Liraglutide, Tirzepatide, and Retatrutide on diabetic kidney disease in db/db mice. Endocrine, 87(1), 159-169.
https://doi.org/10.1007/s12020-024-03998-8
Rosenstock, J., Frias, J., Jastreboff, A. M., Du, Y., Lou, J., Gurbuz, S., … & Coskun, T. (2023). Retatrutide, a GIP, GLP-1 and glucagon receptor agonist, for people with type 2 diabetes: a randomised, double-blind, placebo and active-controlled, parallel-group, phase 2 trial conducted in the USA. The Lancet, 402(10401), 529-544.
 LinkPeptide
LinkPeptide