Proline to the Rescue: How Engineered Peptides Are Redefining SARS-CoV-2 Inhibition
Abstract
As SARS-CoV-2 variants continue to challenge the effectiveness of existing vaccines and therapeutics, the search for innovative antiviral strategies has turned to peptides—especially those targeting host cell entry mechanisms. ATN-161, a pentapeptide that inhibits viral binding to α5β1 integrins, offers a promising foundation but suffers from limited stability and moderate efficacy. In this blog, we explore a recent study that reengineers ATN-161 through proline substitution to enhance its antiviral properties. Among three synthesized analogues, Analogue III (Ac–PHSPN–NH2) demonstrated superior performance, achieving a ~100-fold reduction in viral RNA and the lowest IC50 value in vitro. Molecular docking and dynamics simulations confirmed its strong, stable interactions with both α5β1 integrin and ACE2. With minimal cytotoxicity and enhanced structural integrity, Analogue III stands out as a compelling candidate for further preclinical development. This work highlights the power of peptide engineering to unlock new frontiers in fusion inhibition and viral entry blockade.
The Antiviral Arms Race: Why New Solutions Are Urgently Needed
As the world adapts to life after the peak of the COVID-19 pandemic, SARS-CoV-2 remains a persistent threat. Despite the global rollout of vaccines and the approval of antiviral drugs like Remdesivir, Molnupiravir, and Paxlovid, treatment outcomes are still hampered by viral resistance, reduced efficacy against emerging variants, and narrow therapeutic windows.
This evolving landscape has spotlighted the urgent need for alternative antiviral strategies-particularly those capable of blocking the virus before it even enters human cells. Among the most promising candidates are antiviral peptides: small, tunable molecules that can disrupt key stages of the viral life cycle with remarkable precision.
One such peptide, ATN-161, originally designed for cancer therapy, has shown potential as a fusion inhibitor targeting integrin-mediated viral entry. But researchers are now asking: can we make it even more potent, more stable, and more effective?
The answer may lie in a strategic tweak to its molecular architecture—through the smart use of proline substitution.
Beyond ACE2: The Hidden Role of Integrins in COVID-19 Infection
Much of the early focus on SARS-CoV-2 centered around its now-famous receptor: angiotensin-converting enzyme 2 (ACE2). The virus’s Spike (S) protein latches onto ACE2 to gain entry into host cells-a mechanism now well-documented and heavily targeted in vaccine and drug design.
But ACE2 is not the virus’s only doorway. Mounting evidence suggests that integrins, especially α5β1, play a pivotal supporting role. These transmembrane proteins normally mediate cell adhesion and signaling, but they can also facilitate viral entry by binding to an Arg-Gly-Asp (RGD) motif found in the Spike protein’s receptor-binding domain.
This secondary interaction can stabilize viral attachment, promote membrane fusion, and even amplify inflammatory signaling-making integrins both accomplices in infection and contributors to COVID-19’s vascular complications. Targeting this co-receptor pathway opens up new therapeutic opportunities.
Enter ATN-161, a pentapeptide that binds α5β1 integrin and blocks this viral shortcut—but not without limitations in potency and biochemical stability.
Rewriting the Code: Proline-Based Engineering of ATN-161 Analogues
ATN-161 (Ac–PHSCN–NH2), a five-amino-acid peptide originally developed to inhibit tumor growth, has recently found new purpose as a fusion inhibitor for SARS-CoV-2. By binding to α5β1 integrins, it interferes with viral attachment and may even destabilize the Spike-ACE2 interaction. However, like many short peptides, ATN-161 faces two critical challenges: limited biochemical stability and suboptimal binding strength.
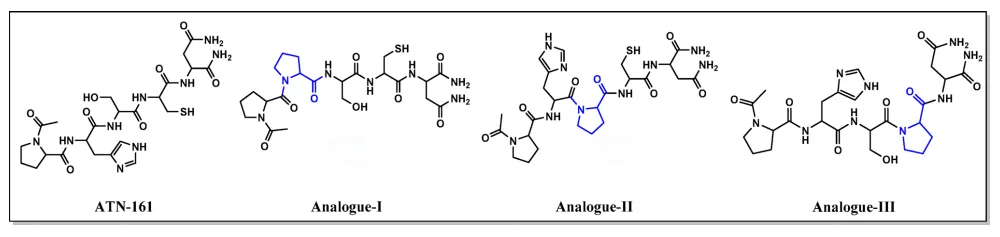
To overcome these hurdles, researchers explored a targeted redesign of ATN-161’s sequence-focusing on proline substitution. Why proline? Its rigid, cyclic structure helps lock peptides into stable conformations, reduces degradation by proteases, and often enhances receptor binding. The team synthesized three new analogues of ATN-161, each featuring a single amino acid swap for proline:
- Analogue I (Ac-PPSCN-NH2): Histidine replaced by proline
- Analogue II (Ac-PHPCN-NH2): Serine replaced by proline
- Analogue III (Ac-PHSPN-NH2): Cysteine replaced by proline
Each variant retained the critical N-terminal acetylation and C-terminal amidation–modifications known to improve peptide half-life and bioavailability. The goal was clear: enhance the peptide’s rigidity, receptor affinity, and antiviral performance without compromising safety.
Next came the real test—how these structural tweaks would perform in biological and computational assays.
Peptides Under Pressure: Synthesis, Screening, and Cell-Based Testing
To evaluate the therapeutic potential of the newly designed ATN-161 analogues, the researchers employed a comprehensive strategy combining synthetic chemistry, in vitro virology, and computational modeling.
Using solid-phase peptide synthesis (SPPS), each analogue was assembled step by step on a Rink Amide resin, ensuring precise sequence control and clean amidation at the C-terminus. Following purification by reversed-phase HPLC and structural confirmation via mass spectrometry and NMR, the peptides were ready for biological testing.
The team turned to Vero E6 cells, a standard model for SARS-CoV-2 infection studies due to their high ACE2 and α5β1 expression. Cells were treated with various peptide concentrations and infected with SARS-CoV-2. After 48 hours, viral replication was quantified via RT-qPCR, and cytopathic effects were examined under phase-contrast microscopy.
Importantly, MTT assays showed no cytotoxicity at concentrations up to 500 µg/mL for any of the analogues-an essential safety signal.
Each analogue was tested alongside the original ATN-161 to directly compare efficacy. The focus wasn’t just on viral inhibition, but also on preserving cell morphology and integrity-key indicators of therapeutic promise.
What emerged from these experiments was a clear winner—one analogue that consistently outperformed the rest across all assays.
Analogue III Emerges as a Potent Viral Fusion Blocker
Among the three engineered analogues, Analogue III (Ac–PHSPN–NH2) stood out as a clear frontrunner. In Vero E6 cell cultures infected with SARS-CoV-2, this variant delivered a dramatic ~100-fold reduction in viral RNA load, with an IC50 of just 0.6 µM. That’s more than five times more potent than the original ATN-161, which clocked in at an IC50 of 3.16 µM.
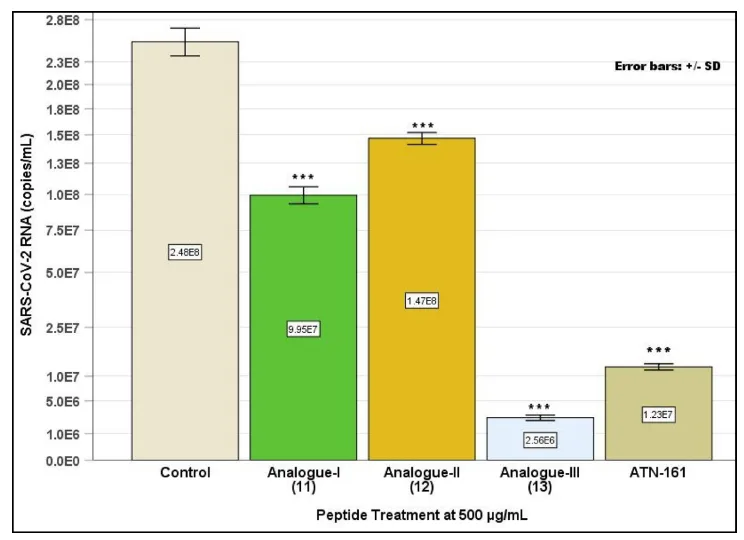
Microscopy revealed that cells treated with Analogue III maintained healthy, intact monolayers-a stark contrast to the shrunken, aggregated, and damaged cells seen in untreated controls. Even at lower concentrations, the peptide exhibited noticeable antiviral activity without any observable cytotoxic effects.
What makes Analogue III so effective? The proline substitution at position 4 (replacing cysteine) appears to offer the perfect balance: enhanced conformational rigidity, reduced oxidative instability, and preserved polar interactions via the remaining histidine and serine residues. These features likely optimize the peptide’s binding to α5β1 integrins and stabilize its antiviral conformation.
In comparison, Analogues I and II showed only modest viral inhibition-even at high concentrations-and were far less effective in preserving cellular morphology.
Clearly, Analogue III isn’t just a minor tweak-it’s a meaningful leap forward in peptide-based antiviral design.
Locking the Gate: How Analogue III Targets Integrins and ACE2
Understanding why Analogue III outperformed its peers required a closer look at the molecular level. The research team turned to molecular docking simulations, targeting two key viral entry points: the α5β1 integrin (both open and closed conformations) and the ACE2 receptor.
Docking scores revealed the strength of each peptide’s binding. Analogue III exhibited the most favorable docking energies across all targets, with a standout −17.05 kcal/mol score against the open conformation of α5β1 integrin. It also maintained low RMSD values (as low as 1.113 Å), indicating stable and precise fits in the receptor binding pockets.
The peptide formed strong interactions with critical residues-particularly Asp227, Asp228, Leu257, and Lys254-known to be essential for Spike-integrin engagement. Similar binding was observed with ACE2, where Analogue III interacted with residues like Gln102, Asp206, and Glu398, contributing to a secondary layer of viral entry blockade.
These results confirm that the enhanced in vitro performance of Analogue III is rooted in its superior molecular affinity and structural stability. By reinforcing both the integrin and ACE2 interfaces, this engineered peptide acts as a dual-entry inhibitor-an uncommon and valuable feature for antiviral agents.
Stability in Motion: What Molecular Dynamics Reveal
Docking provides a snapshot-but molecular dynamics (MD) simulations reveal how peptide–receptor interactions hold up over time under physiological conditions. Over a 100-nanosecond simulation, Analogue III formed remarkably stable complexes with α5β1 integrin, especially in its open conformation.
Compared to ATN-161, which showed more fluctuations and binding flexibility, Analogue III maintained low and consistent RMSD values throughout the simulation. This indicates a tight, well-fitting interaction with minimal structural drift-exactly what’s needed for reliable therapeutic action.
While flexibility can sometimes benefit a ligand, in this case, rigid, stable binding seems to translate directly to improved viral inhibition. Analogue III’s conformation isn’t just effective-it’s durable.
Peptides with Purpose: Why Analogue III Matters Beyond COVID-19
Analogue III represents more than just an incremental improvement-it’s a proof of concept for how strategic peptide engineering can elevate a molecule from modest to exceptional. By preserving key polar residues like histidine and serine, while replacing cysteine with proline, the analogue achieves greater biochemical stability without sacrificing target specificity.
This approach could extend beyond SARS-CoV-2. The success of Analogue III underscores the potential of integrin-targeted peptides as a therapeutic class-offering a flexible platform for countering not only viral infections but also other integrin-mediated pathologies like inflammation and cancer.
Blueprint for the Future: What Analogue III Teaches Us About Antiviral Design
While the results are promising, they come with caveats. The antiviral effects of Analogue III were tested in Vero E6 cells, which lack the TMPRSS2 protease found in human respiratory epithelium. Moreover, in silico ADMET predictions must be verified through real-world pharmacokinetic and toxicity studies.
The next steps are clear: conduct in vivo validation, explore human cell models, and develop optimized delivery methods-such as intranasal or inhalable formulations-to fully unlock the therapeutic potential of this peptide.
The redesign of ATN-161 into Analogue III demonstrates how thoughtful molecular engineering can transform a promising lead into a next-generation antiviral. By enhancing stability, specificity, and integrin-targeting efficiency, this proline-modified peptide offers a novel route to fusion inhibition-not just for SARS-CoV-2, but potentially for future viral threats as well.
Reference
Munawar, M., Khan, N. U. H., Jabeen, S., Taj, S., Bashir, R., Abbas, W., … & Iqbal, M. (2025). Design and Evaluation of ATN-161 Analogues as Fusion Inhibitors Targeting Integrins in SARS-CoV-2. International Journal of Peptide Research and Therapeutics, 31(4), 1-25.
https://doi.org/10.1007/s10989-025-10734-x
Luna, O. F., Gomez, J., Cárdenas, C., Albericio, F., Marshall, S. H., & Guzmán, F. (2016). Deprotection reagents in Fmoc solid phase peptide synthesis: moving away from piperidine?. Molecules, 21(11), 1542.
https://doi.org/10.3390/molecules21111542
Lan, J., Ge, J., Yu, J., Shan, S., Zhou, H., Fan, S., … & Wang, X. (2020). Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor. nature, 581(7807), 215-220.
 LinkPeptide
LinkPeptide