Targeting Alpha-Synuclein: KEQPTN Peptide Offers New Hope in Parkinson’s Disease Therapy
Abstract
Parkinson’s disease (PD) is characterized by the pathological aggregation of alpha-synuclein, particularly within its hydrophobic NAC region, leading to the formation of toxic fibrils and Lewy bodies. This study presents the rational design and evaluation of a synthetic peptide inhibitor, KEQPTN, aimed at disrupting alpha-synuclein fibrillization. A peptide library was constructed through targeted point mutations to enhance hydrophilicity and reduce aggregation propensity. KEQPTN emerged as a lead candidate based on in silico screening, including toxicity prediction, cell penetration, blood-brain barrier permeability, and molecular docking. Molecular dynamics simulations demonstrated stable binding and favorable energetics with the NAC region. Subsequent in vitro assays, including Thioflavin T fluorescence and MTT cytotoxicity tests on SH-SY5Y cells, confirmed KEQPTN’s ability to inhibit fibril formation and reduce alpha-synuclein-induced toxicity. These findings position KEQPTN as a promising peptide-based therapeutic candidate and support further investigation into peptide inhibitors as disease-modifying strategies for PD.
Alpha-Synuclein and the Molecular Origins of Parkinson’s Disease
Parkinson’s disease (PD) is a progressive neurodegenerative disorder affecting over 10 million people globally. While commonly recognized for its motor symptoms—tremors, rigidity, and bradykinesia—PD also involves a deeper pathological process rooted in the selective loss of dopaminergic neurons in the substantia nigra. This neuronal degeneration severely disrupts motor control and contributes to non-motor complications such as cognitive decline and depression.
A major molecular hallmark of PD is the accumulation of alpha-synuclein, a presynaptic neuronal protein that normally regulates synaptic vesicle dynamics. In disease states, alpha-synuclein misfolds and aggregates into insoluble fibrils, forming Lewy bodies—intracellular inclusions that are characteristic of PD and related synucleinopathies.
Of particular importance is the non-amyloid-β component (NAC) region of alpha-synuclein, encompassing residues 61 to 95. This hydrophobic core is critical for fibril nucleation and beta-sheet formation, making it a central focus in efforts to block pathological aggregation. Understanding how to modulate the structural behavior of this region is key to developing effective molecular inhibitors that can potentially interfere with disease progression at its root.
Engineering Interference: Designing a Peptide to Target the NAC Domain
Given the central role of alpha-synuclein aggregation in Parkinson’s disease, therapeutic strategies have increasingly focused on disrupting this process at its origin. In this context, the NAC region—highly hydrophobic and intrinsically aggregation-prone—presents a logical molecular target.
The study in focus applied a biomimetic design strategy to develop peptide-based inhibitors specifically targeting the NAC domain. Drawing from the sequence of residues 60–70 within alpha-synuclein (KEQVTNVGGAV), researchers generated a library of over 100 six-residue peptide variants by introducing point mutations to increase hydrophilicity. This substitution approach—replacing nonpolar amino acids with polar or charged residues—was intended to reduce the region’s aggregation potential by enhancing its solubility and disrupting beta-sheet formation.
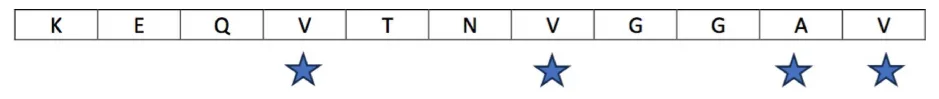

Each peptide candidate underwent rigorous in silico screening using multiple bioinformatics tools:
- ToxinPred and AlgPred to eliminate toxic or allergenic sequences
- BChemRF-CPPred for assessing cell-penetrating potential
- BBB Predictor for blood-brain barrier permeability
- HADDOCK docking simulations to evaluate binding affinity with alpha-synuclein fibrils
From this multi-step computational triage, four lead peptides emerged—among them, a standout sequence: KEQPTN. The presence of proline, known to disrupt secondary structures, was a defining feature that contributed to reduced aggregation propensity.
KEQPTN was not only predicted to bind effectively to the aggregation interface but also showed high hydrophilicity, non-toxicity, and favorable uptake and penetration profiles. These properties positioned it as a strong candidate for experimental validation in both structural and cellular models of alpha-synuclein aggregation.
From Code to Chemistry: Simulations and Experimental Validation of KEQPTN
After computational screening established KEQPTN as the most promising candidate, the researchers moved into experimental validation to test whether the peptide could truly interfere with alpha-synuclein fibrillization. This phase combined molecular dynamics simulations, structural assays, and cell-based toxicity studies, offering a comprehensive evaluation of KEQPTN’s behavior in silico and in vitro.
Molecular Dynamics Simulation
Using the GROMACS platform, 100-nanosecond molecular dynamics (MD) simulations were performed to assess the peptide’s interaction with alpha-synuclein fibrils. KEQPTN demonstrated superior structural stability, indicated by its low Root Mean Square Deviation (RMSD) and compact radius of gyration (Rg). Importantly, the peptide consistently formed 3–6 stable hydrogen bonds with the NAC region of alpha-synuclein, particularly residues Thr72, Ser87, and Ala90—key sites involved in fibril formation.
Binding Affinity and Energy Profile
Further analysis using MM-PBSA (Molecular Mechanics/Poisson–Boltzmann Surface Area) calculations revealed a favorable total binding energy of −33.4 kJ/mol for the KEQPTN–alpha-synuclein complex. This result reflected strong van der Waals and electrostatic interactions that effectively countered the solvation penalty—an essential balance for stable, specific binding.
Biochemical Validation
The peptide was then synthesized via solid-phase synthesis, purified using HPLC (99.67% purity), and structurally confirmed via LC–MS. Functional testing began with the Thioflavin T (ThT) assay, a standard method for monitoring beta-sheet-rich fibril formation. KEQPTN significantly reduced ThT fluorescence in a dose-dependent manner, especially between 50–70 µM concentrations, indicating robust inhibition of fibril growth.
Complementing this, fluorescence microscopy visually confirmed a striking reduction in fibril formation, while MTT assays on SH-SY5Y neuronal cells revealed that KEQPTN not only mitigated cytotoxicity induced by alpha-synuclein aggregates but also restored cell viability to near-normal levels.
Interrogating the Data: Limitations, Caveats, and Future Directions
Despite the promising results, the study also underscores several limitations that must be addressed before KEQPTN can progress toward clinical relevance.
Firstly, while the Thioflavin T assay clearly indicated fibril inhibition, this fluorescence-based method provides only indirect evidence of structural changes. It does not distinguish between classical amyloid fibrils and other ThT-binding aggregates. Therefore, the authors note the importance of complementary structural techniques—such as transmission electron microscopy (TEM) or circular dichroism (CD) spectroscopy—to directly observe changes in aggregate morphology and secondary structure.
Secondly, the incubation time for fibril formation was limited to 24–48 hours, a timeframe that captures early aggregation events but may not reflect the full dynamics of fibril growth over time. Extended assays and kinetic modeling will be essential to validate KEQPTN’s long-term efficacy.
Third, while the peptide showed good cell penetration and low toxicity in vitro, in vivo stability remains a challenge. Like many short peptides, KEQPTN is potentially vulnerable to rapid degradation by proteases. To address this, the authors suggest future modifications such as cyclization, terminal acetylation/amidation, or incorporation of D-amino acids to enhance half-life and bioavailability.
Overall, these limitations do not diminish the significance of the findings but rather define the logical next steps toward therapeutic translation.
Peptide Therapeutics and the Promise of Disease Modification in PD
The development and validation of KEQPTN signal a compelling advance in the evolving strategy to treat Parkinson’s disease at the molecular level. Unlike current therapies, which primarily focus on managing symptoms through dopamine replacement or neuromodulation, peptide-based inhibitors like KEQPTN target the upstream pathology—namely, the misfolding and aggregation of alpha-synuclein.
By specifically binding to the NAC region and disrupting the structural motifs necessary for fibril formation, KEQPTN offers a disease-modifying mechanism that could halt or slow the progression of PD. Just as importantly, its demonstrated ability to reduce alpha-synuclein-induced cytotoxicity suggests a dual benefit: not only preventing fibril accumulation but also protecting neurons from toxic intermediates, such as soluble oligomers.
While substantial work remains—including pharmacokinetics, delivery optimization, and long-term in vivo validation—this research highlights the power of rational peptide design in tackling complex neurodegenerative processes. It also illustrates the value of integrated workflows that combine bioinformatics, structural modeling, and wet-lab validation.
In the broader context of neurodegenerative disease research, KEQPTN represents more than a single molecule—it marks a shift toward targeted, mechanism-based therapies capable of addressing the root causes of protein misfolding disorders.
Reference
Jabbari, A., Niknejad, A., Allahyarifard, N., Karami, L., & Motamedi, M. (2025). Development of a Peptide Inhibitor To Prevent Alpha-Synuclein Fibrillization in Parkinson’s Disease. International Journal of Peptide Research and Therapeutics, 31(4), 1-19.
https://doi.org/10.1007/s10989-025-10728-9
Angelopoulou, E., Paudel, Y. N., Papageorgiou, S. G., & Piperi, C. (2022). Environmental impact on the epigenetic mechanisms underlying Parkinson’s disease pathogenesis: a narrative review. Brain Sciences, 12(2), 175.
https://doi.org/10.3390/brainsci12020175
Wang, L., Wang, N., Zhang, W., Cheng, X., Yan, Z., Shao, G., … & Fu, C. (2022). Therapeutic peptides: current applications and future directions. Signal transduction and targeted therapy, 7(1), 48.
 LinkPeptide
LinkPeptide